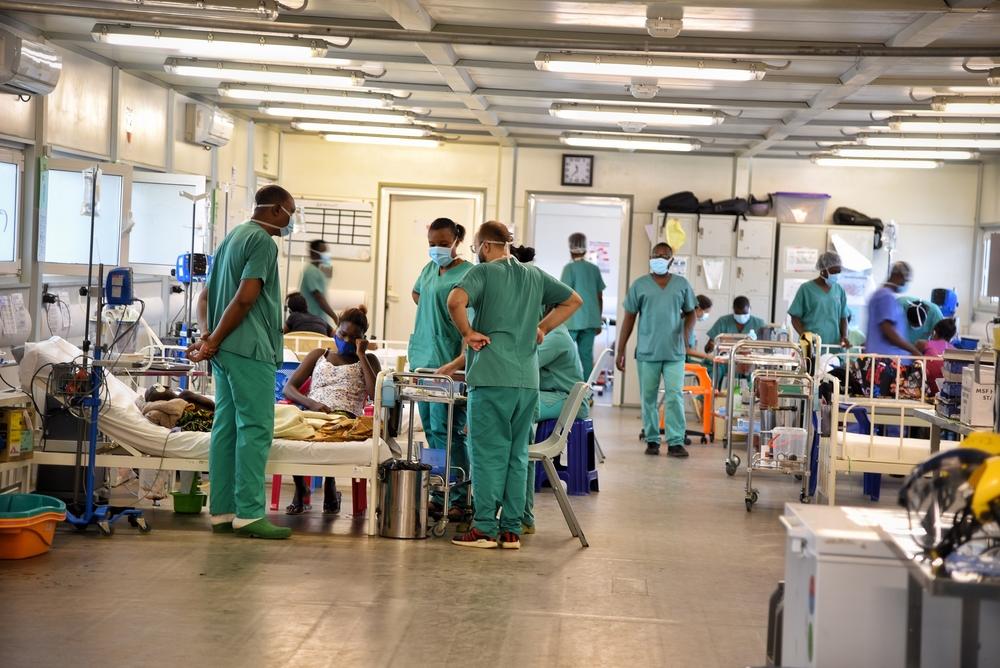
A rising tide of antimicrobial resistance (AMR) is jeopardizing hard-won healthcare progress in Sierra Leone, according to a new report. The study warns that drug-resistant infections are threatening to roll back the gains made in fighting infectious diseases nationwide.
The report highlights alarming trends in hospitals across Freetown, where routine use of empirical antibiotic prescriptions far exceeds WHO recommendations. At Connaught Hospital, two‑thirds of inpatients received antibiotics—with an average of two different drugs per patient—often without laboratory testing or prescription justification. This is in contrast with the WHO benchmark of below 30% antibiotic use in similar settings .
Further investigations revealed widespread resistance among key pathogens. At least 58% of isolates were extended-spectrum beta-lactamase (ESBL) producers, while carbapenem-resistant organisms and methicillin-resistant Staphylococcus aureus (MRSA) were also detected at non-negligible levels. These findings highlight a critical threat to treatment effectiveness .
Compounding the crisis, a continent-wide assessment by Africa CDC and the African Society for Laboratory Medicine found that Sierra Leone’s capacity for AMR surveillance remains extremely limited. Of the priority pathogens identified by WHO, consistent testing is conducted for only a handful. Shockingly, barely 1% of laboratories in the surveyed countries—including Sierra Leone—conduct bacteriology testing at all, severely constraining public health response .
In the agriculture and animal health sector, resistance is also escalating. A recent FAO‑supported study in the poultry industry revealed extremely high resistance rates—E. coli showed resistance to sulfamethoxazole in nearly 90% of samples, while Salmonella exhibited rates above 94%. These findings point to growing AMR risks within agriculture and animal‑human interfaces .
Health experts emphasise that without stronger antibiotic stewardship programs, better laboratory infrastructure, and improved diagnostic capacity, AMR may derail national progress toward Sustainable Development Goals. Sierra Leone’s previous AMR strategic plan (2018–2022), though well-designed, lacked full implementation due to inadequate budgeting and coordination .
The report concludes with urgent recommendations:
• Establish and fully resource antimicrobial stewardship committees in hospitals.
• Expand and operationalize national AMR surveillance through laboratory capacity–building.
• Strengthen enforcement and regulation in both human health and agricultural settings.
• Continue multisectoral coordination under a One Health framework.
Without rapid, sustained action, Sierra Leone risks facing a resurgence in infectious disease mortality—potentially reversing years of healthcare gains.
By Julliet Amara